Cancer
Welcome to Stronach Regional Cancer Centre
-
Welcome
-
News & Media
-
Contact
-
Patients and Families
-
Resources
-
Survivorship
-
Central Regional Cancer Program
-
Healthcare Providers
-
Physician Directory
-
Programs & Clinics
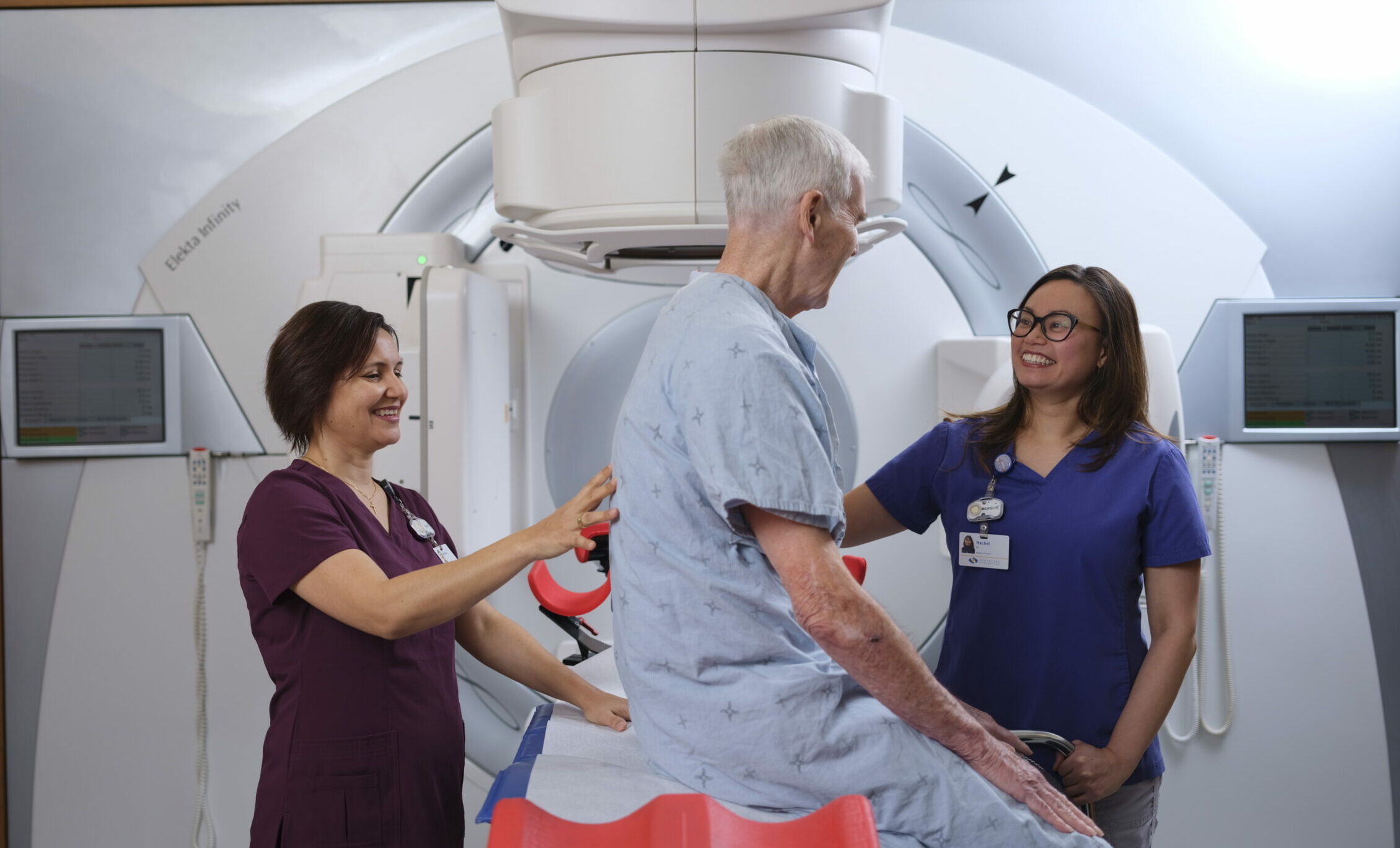
Welcome to the Stronach Regional Cancer Centre (SRCC) at Southlake, which represents the regionally designated program for the Central Regional Cancer Program. We compassionately deliver programs and services for patients living in York Region, North York and South Simcoe County, including cancer screening, diagnostic testing, radiation, chemotherapy and supportive care. Southlake’s cancer program includes both inpatient and outpatient services and the two areas work together to provide seamless care. Our staff are by your side every step of the way.
Informed by innovative research, our oncology experts provide excellent, closer to home care in our state-of-the-art treatment facility. We co-lead shared-care cancer programs with renowned partners such as Princess Margaret Cancer Centre and SickKids Hospital.
As the regional hub, we help to inform our region’s hospitals, cancer clinics, other service providers and family physicians of new information, tools and programs from Ontario Health-Cancer Care Ontario to help deliver high quality, safe cancer care.
Top 10 symptom management documents
- Anxiety
- Depression
- Diarrhea
- Exercise
- Fatigue
- Fever
- Loss of Appetite
- Nausea and Vomiting
- Pain
- Sexual Health
All available Ontario Health – Cancer Care Ontario Symptom Management Documents can be found at the following link: https://www.cancercareontario.ca/en/symptom-management
Patient Information Guide

Find Southlake
Referral Forms
Preparing for Care
Donate
Parking at Southlake
Southlake Visitor Guidelines
Amenities for Patients & Visitors
News
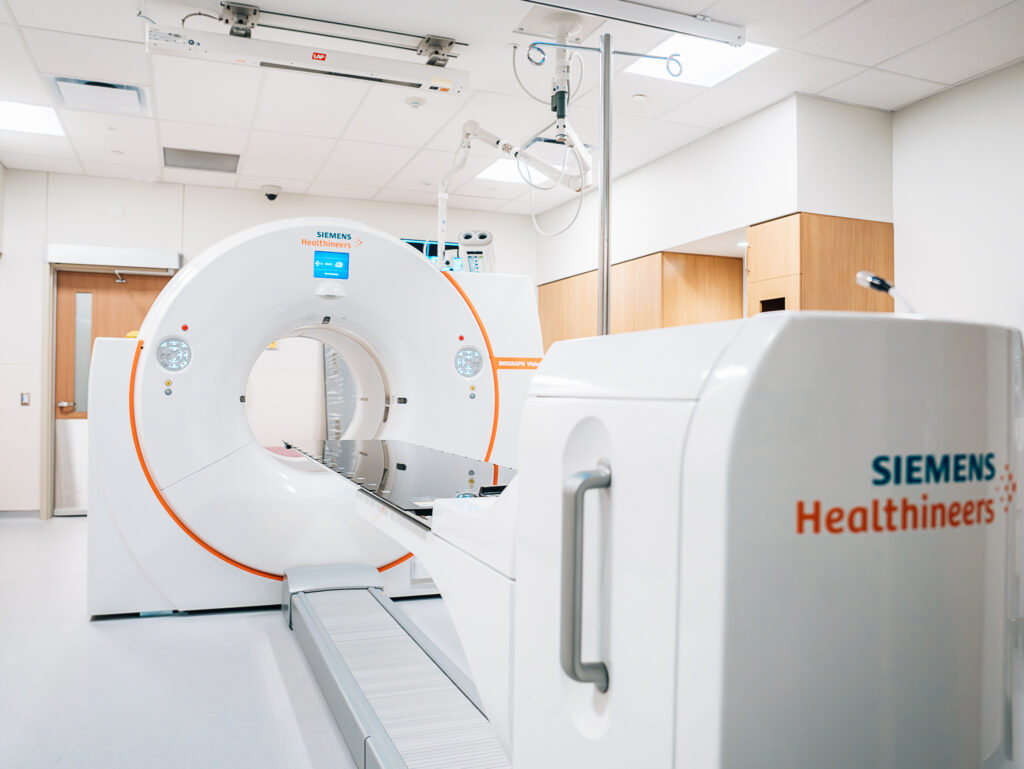
First PET-CT scanner in York Region opens at Southlake
Monday September 18, 2023
To reach the Stronach Regional Cancer Program at Southlake – call 905-830-5800 and follow the prompts listed below. If your call is regarding a prescription refill, please have your pharmacy fax us a refill request a few days before your medication runs out to 905-952-3053.
- To confirm, book, change or cancel an appointment, PRESS 1
- This includes:
- Treatment appointments, like Chemotherapy, Radiation or Supportive Treatments (like transfusion or hydration).
- Nurse or Doctor appointments.
- Lab appointment
- CT scan, Ultrasounds, or any other tests
- Radiation Planning appointments.
- Psychosocial Oncology appointments, like Social Work, Dietician, Medical Psychotherapy or Psychiatry.
- Palliative Clinic appointment.
- To obtain medical forms or release of information PRESS 2
- To contact the referrals office PRESS 3
- Questions about your referral
- If you have a symptom management related question PRESS 4
- This includes:
- Any symptoms related to your treatment – Radiation or Chemotherapy
- This includes:
Attending your first appointment at the Stronach Regional Cancer Centre is a key step in your experience with cancer. You should plan to stay for two to four hours. During this time, you will meet with some members of your care team, who will review your medical history and arrange any tests you may need.
To prepare for your first visit, review these checklists.
For family members or friends caring for an adult or child with cancer, here are several ways you can help your loved one during this experience.
- Attend appointments with them. We encourage our patients to bring a caregiver, family member or friend to their first visit and subsequent appointments with their care team. As our patients receive a lot of information during these visits, you can help take notes and review information together after the appointment.
- Ask questions. Please make a list of your questions and bring them with you to your family member or friend’s appointments. We want to ensure our patients and their caregivers have the information they need.
- Help them find answers. You may want to do some of your own research and discuss the answers you find with your family member or friend’s care team. Visit our Patient & Family Resource Centre, which is located next to the Welcome Centre reception desk on the Lobby level. Open and staffed by trained volunteers, from Monday to Friday, 9 a.m. to 4 p.m., it provides free access to current, reliable and accurate health information and internet access.
Click here to view our patient information guide.
Watch the video below for what to expect at your first visit.
COVID-19 and cancer – click here for information and resources.
Patient & Family Resource Centre
A key part of your patient experience is to be informed. Any question is worth asking and our staff is available to answer them at your convenience. To support your search for information, we encourage you to visit our Patient & Family Resource Centre, which is located next to the Welcome Centre reception on the Lobby level.
Open and staffed by trained volunteers, from Monday to Friday, 9 a.m. to 4 p.m., it provides free access to current, reliable and accurate health information and internet access. They can be reached by phone at 905-895-4521 ext. 6051, or by email at PFRC@southlake.ca.
The Healing Garden
The Healing Garden is located on the west side of the Cancer Centre. You can get to it from the Prospect Street exit, on the Lobby level or through the Radiation Therapy Department on the Ground level. It is a large area with flowers, trees, a fountain and benches and is a quiet, calm place to spend time.
The Quiet Room
We also have a Quiet Room for patients, family, staff and volunteers. It is located on Level 1, near the main elevators. Patients can use this room for quiet reflection, prayer and meditation.
Indigenous Resources
Southlake and the Stronach Regional Cancer Centre (SRCC) are committed to actively participating in the truth and reconciliation process. We are pleased to share that SRCC now has a process in place to allow patients to perform a Smudging ceremony on-site. When you visit the cancer centre, please let your healthcare provider know that you wish to Smudge and they will happily accommodate your request. You are more than welcome to bring your own Smudging materials, or they will be available on-site by request.
General
- Central Regional Indigenous Cancer Plan: coming soon
- BANAC Aging-at-Home Program, South Simcoe and York Region
- ICCU First Nations, Inuit, Métis and Urban Indigenous Cancer Strategy 2019–2023
- Cancer 101 Toolkit for First Nations, Inuit & Métis People
- Silent Enemy – Comic About Cancer Diagnosis, Treatment and Recovery
- Vaping and Your Health for First Nations, Inuit, Métis and Urban Indigenous Peoples
- Cannabis and Cancer for First Nations, Inuit, Métis and Urban Indigenous Peoples
- Indigenous Tobacco Program: Tobacco-Wise Resources for Indigenous Community Members
- Canadian Virtual Hospice – LivingMyCulture.ca
- Palliative Care Toolkit – Cancer Care Ontario
First Nations
- Cancer in First Nations in Ontario – Risk Factors and Screening
- Be Tobacco-Wise: The Benefits of Quitting Smoking (First Nations)
- First Nations Breast Screening Fact Sheet
- First Nations Colon Cancer Screening Fact Sheet
- First Nations Cervical Screening Fact Sheet
Métis
- Be Tobacco-Wise
- Métis Breast Screening Fact Sheet
- Métis Cervical Screening Fact Sheet
- Métis Colon Screening Fact Sheet
Inuit
Programs for you
As a cancer survivor finished your active cancer treatment, you may have lingering questions, concerns and needs. Am I doing the right things? How can I manage new medical challenges? Will my cancer return?
Pathways to wellness
At the Stronach Regional Cancer Centre (SRCC) at Southlake, we offer the Pathways to Wellness program, which is a free, evidence-based community program, open to cancer survivors who have completed their treatment. This six-week program offers weekly, two-hour sessions that include group support, exercise and discussions to give you information and strategies to help you:
- Manage your stress and anxiety,
- Improve your nutrition,
- Maximize your physical activity
- Manage your health concerns
For more information or to register, contact Adriana Quercia, 905-830-5800 ext. 6536.
Help to find support groups and resources
Stop by our Patient and Family Resource Centre located in the Lobby of SRCC (near the Welcome Centre) or speak to a member of the healthcare team so we can help you find support that meets your needs.
Additional tools:
You may also want to check the following external programs for additional support:
For all cancers:
- Canadian Cancer Society: Life After Cancer (online information and supports)
- Cancer Bridges (resources for cancer survivors)
- Cancer Care Ontario
- Canadian Cancer Society (Information on all types of cancer and services for patients and families)
- Cancer Chat Canada (professionally led online support groups for Canadians affected by cancer)
- Cancer and Work Canada (helps cancer survivors with returning, remaining, changing work or looking for work after their diagnosis)
For breast cancer:
- Life After Breast Cancer (breast cancer transition)
- Canadian Breast Cancer Foundation
- BRA Day (breast reconstruction)
- My Reconstruction
For other specific cancers:
Central Regional Cancer Program
The Central Regional Cancer Program delivers full-service cancer care through a network of hospital partners and other service providers to help you stay healthy. We host a range of programs, including prevention and screening community education activities, hospice palliative care outreach, and physician support, all of which support other healthcare professionals throughout the region.
All of our partner hospitals and cancer care centres have partnership agreements with Ontario Health-Cancer Care Ontario. Each hospital provides various aspects of cancer care, such as medical oncology, chemotherapy and palliative care, but the Stronach Regional Cancer Centre at Southlake is the only centre to provide radiation oncology in the Central Region.
Our hospitals and cancer centre services work with support from other service providers, such as public health units, family health teams and family practitioners, community agencies, Home and Community Care Services, and hospices.
Select each hospital image below to learn about the cancer services and programs it offers.
- Humber River Hospital
- Mackenzie Health
- Markham Stouffville Hospital
- North York General Hospital
- Stevenson Memorial Hospital
Regional Prevention & Screening Program
The Regional Prevention and Screening team aims to increase cancer prevention practices and participation in Ontario’s breast, cervical and colon screening programs. The team also works on smoking cessation for the cancer program so that patients can get the best possible effects from their cancer treatment.
Cancer Prevention
About 4 in 10 cancer cases in Canada can be prevented. There are things we eat, drink, and do that affect our cancer risk. For additional information on each of these topics, please follow the links below:
- Stay smoke-free
- Limit alcohol
- Eat healthy
- Exercise for at least 30 minutes a day
- Get vaccinated against HPV
- Know your risk for cancer
Cancer Screening
Cancer screening testing is done on people who are at risk of getting cancer, but who have no symptoms and generally feel fine. Ontario has three province-wide cancer screening programs: ColonCancerCheck (CCC), the Ontario Breast Screening Program (OBSP), and the Ontario Cervical Screening Program (OCSP).
ColonCancerCheck (CCC): More information on when to get screened, what types of colon cancer screening tests there are, where you can get screened, and other resources.
Ontario Breast Screening Program (OBSP): More information on when to get screened, what a breast cancer screening test is, where you can get screened, and other resources.
Ontario Cervical Screening Program (OCSP): More information on when to get screened, what a cervical cancer screening test is, where you can get screened, and other resources.
If you have questions or need more information, please contact the Prevention and Screening team by email at icsregional@southlake.ca or by phone at 905-895-4521 ext. 6065.
Hospice Palliative Care Team – Pain & Symptom Management in the Community
The Hospice Palliative Care Teams for our region help healthcare providers deliver high quality hospice palliative care to patients, families and caregivers in their homes. Our Clinical Nurse Consultants and Nursing Manager serve as a resource to help healthcare providers interpret and apply assessment tools and best practice guidelines to care. We facilitate hospice palliative care consultations, education, mentorship and support for community palliative care providers.
We participate in regular, interprofessional rounds in the region. These rounds give care teams the opportunity to review patient care plans, make change, and provide education to meet the changing needs of patients and their caregivers.
Click here to view the HPC Team brochure.
To refer a patient to the Stronach Regional Cancer Centre, download, complete and fax the appropriate Referral Form from the list on the right to 905-952-2820.
Southlake is now accepting e-referrals! To refer radiation oncology and medical oncology patients electronically, please click here.
For palliative consultation (forms also located under Requisition and Referral forms to the right), fax the completed form, with any required documents, to 905-830-5978. Alternatively, you may mail the form and documents to: HPC Teams for Central LHIN, 596 Davis Drive, Box 22, Newmarket, Ontario L3Y 2P9
If you have any questions about this service or how to complete these forms, contact the HPC Teams at 905-895-5800 and follow the prompts.
If a requisition/referral form is missing from the sidebar, please click here for a full list.
Education for Health Care Providers
Caring for First Nations, Inuit and Metis Patients
The Central Regional Cancer Program works with Ontario Health-Cancer Care Ontario to implement the Aboriginal Cancer Strategy — a roadmap for addressing the unique cancer care issues affecting First Nations, Inuit and Métis (FNIM) communities.
This strategy includes various resources to help healthcare providers holistically care for these communities, such as the following:
- Aboriginal Cancer Strategy IV is a plan created by Ontario Health-Cancer Care Ontario and FNIM communities to guide work within these communities.
- Aboriginal Relationship and Cultural Competency Courses are free online modules that can increase your knowledge of FNIM cancer care. As you complete these modules, you can earn Mainpro credits.
LEAP Core
Learning Essential Approaches to Palliative (LEAP) and End-of-Life Care Core is Pallium Canada’s two-day program offering competency-based palliative care education for healthcare professionals. This program, led by a LEAP certified facilitator, is based on Canadian realities and current best practice in palliative and end-of-life care.
No prerequisites: This course is only for professionals working in the Central Region. Attendance is mandatory to receive certification and for physicians to receive 26.5 College of Family Physicians of Canada (CFPC) group learning credits.
If you are interested in attending, contact Hospice Palliative Care Teams at 905-895-4521, ext. 6388.
Resources for Health Care Providers
There are a variety of cancer screening decision support tools and resources available to support you in your screening activities.
Breast Screening
- For current breast cancer screening guidelines, visit Ontario Breast Screening Program (OBSP) Guidelines.
- For breast screening locations, including high risk assessment sites, visit Ontario Breast Screening (OBSP) locations.
Colorectal Screening
- For the FIT + Colonoscopy referral form please click here.
- For current colorectal cancer screening guidelines including post-polypectomy surveillance guidelines, visit the Colorectal Cancer Screening Recommendations.
- For access to forms, instructions, FAQs, and other resources related to FIT, visit the FIT Resource Hub.
- As part of the ColonCancerCheck program, patients without a primary care provider are able to be screened. Patients with an abnormal FIT require an urgent colonoscopy. Please consider registering to accept unattached patients requiring this follow-up to your practice. You can register by completing this form.
Cervical Screening
- For the current cervical screening guidelines, visit Ontario Cervical Screening Guidelines.
Cancer Screening Tools and Support for Primary Care Providers
- Screening Activity Report (SAR)
The SAR is an interactive online tool available to primary care physicians who practice as part of a patient enrolment model. It provides screening data for breast, cervical and colorectal cancers to help physicians improve their cancer screening rates and appropriate follow-up. For more information on the SAR, visit www.cancercareontario.ca/SAR. - Physician-Linked Correspondence
Cancer screening letters are a key way to encourage people to be screened. With your physician-linked correspondence enrolment, your rostered patients’ will receive their cancer screening letters (invitation, recall, and reminder letters) sent on your behalf. For more information on PLC and to complete the consent form, visit CCO’s physician-linked correspondence page. - Quality Improvement Project Support to Improve Cancer Screening
- Group Screening Summaries or Individual Screening Summaries available for PEM physicians upon request
- Subscribe to the Central Regional Cancer Program’s Quarterly newsletters with program updates/reminders, information and resources related to cancer prevention and screening.
- For more information, questions, or to sign up for SAR, PLC and/or the newsletters, contact the Prevention and Screening team, Central Regional Cancer Program at icsregional@southlakeregional.org or 905-895-4521 ext. 6065
Cancer Care Ontario E-Learning
- Cancer Care Ontario offers accredited courses online to better serve the healthcare community. Available 24 hours a day, the website offers MainPro+ accredited Indigenous cultural awareness courses. For more information, click here.
Annual Central Region Oncology Day for Primary Care Providers
As the designated regional program for the Central Regional Cancer Program, the Stronach Regional Cancer Centre at Southlake invites primary care providers and its community partners to participate in a conference every year for Oncology Day. Click here to view the 2020 brochure.
Requisition & Referral Forms
Filter by Name
Filter by Department
Filter by Language
Dr. Zishan Allibhai
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Peter Anglin
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Arnell Baguio
Palliative Care Physicians
Family & Community Medicine/CMR/Palliative Care
(905) 895-4521
English
Dr. Elaine Bouttell
Medical Oncologists
Medical Oncologist
905-895-4521
English
Dr. Charles Cho
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Tatiana Conrad
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Sophia Farooki
Medical Oncologists
Hematologist
(905) 895-4521
English
Dr. Louis Fenkell
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Jai Jayakar
Internal Medicine
Hematologist/Medical Oncologist
905-895-4521
English
Dr. Farrah Kassam
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Shaqil Kassam
Medical Oncologists
Medical Oncologist
905-895-4521
English
Dr. Fatma-Zahra Kassam
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Adrianne Lebner
Palliative Care Physicians
Family & Community Medicine/CMR
(905) 895-4521
English
Dr. Cynthia Luk
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Koushalya Paramsothy
Medical Oncologists
Hematologist
(905) 895-4521
English
Dr. Yasmin Rahim
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Amira Rana
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Allison Ransom
Palliative Care Physicians
Family & Community Medicine/CMR
(905) 775-8782
English
Dr. Demetrios Simos
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Dr. Cindy So
Palliative Care Physicians
Family & Community Medicine/CMR
(905) 895-4521
English
Dr. Kimberly Sutton
Palliative Care Physicians
Family & Community Medicine/CMR
(905) 476-3775
English
Dr. Mojgan Taremi
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Woodrow Wells
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Jason Wong
Radiation Oncologists
Radiation Oncologist
(905) 895-4521
English
Dr. Harold Yuen
Palliative Care Physicians
Family & Community Medicine/CMR
(905) 895-4521
English
Dr. Labib Zibdawi
Medical Oncologists
Medical Oncologist
(905) 895-4521
English
Adolescent and Young Adult (AYA) Program
Adolescent and Young Adult (AYA) Program
The Adolescent and Young Adult (AYA) Program at Southlake provides personalized, supportive care to young adults with cancer. This program is a partnership between Southlake and University Health Network (UHN).
We provide the following supportive care:
- Family support
- School/work
- Sleep support
- Coping and wellness
- Rehabilitation
- Sexual health and fertility
- Peer connection
- Nutrition
For more information contact AYA@southlake.ca.
Chemotherapy Program Clinic
Chemotherapy Program Clinic
Chemotherapy (chemo) is a treatment that uses drugs to damage and stop cancer cells from growing. You can take chemo drugs as a pill (orally), by injection with a needle or into your vein (intravenously). The cancer’s location, treatment goal, type of drug and other factors help your care team decide the best way to give your chemo.
Chemo is usually given in cycles or repeated doses. This means you will receive medication followed by a period of rest, which gives your body time to replace damaged cells and regain strength.
Learn more about chemotherapy in our Chemotherapy 101 video below.
Clinical Trials Program
Clinical Trials Program
Stronach Regional Cancer Centre
Clinical trials are research studies to test new procedures, drugs or equipment that pave the way to advanced practices in cancer detection, treatment and prevention. Through clinical trials, cancer patients and cancer researchers can continue to develop new treatments, care and prevention that enhances our patients’ outcomes and experience. When you participate in a clinical trial, you directly contribute to the global quest for knowledge on how cancer forms and how we can best treat it.
We encourage our patients’ interest and participation in clinical trials.
Diagnostic Assessment Programs/Clinics
Diagnostic Assessment Programs/Clinics
- T 905-895-4521 x 2960
Medical Arts Building, 581 Davis Drive
Your experience with cancer may start when you or your family physician has concerns about your health or a screen test has suspicious results. Our Diagnostic Assessment Program can save you time and reduce your stress by coordinating your tests and appointments, connect you with a Nurse Navigator, and help fast-track services to diagnose breast, colon, lung, prostate or skin cancer.
Palliative Care Program & Clinic
Palliative Care Program & Clinic
Palliative care is a team approach to care that is appropriate for a patient and/or family member living with a life-limiting illness or needing end-of-life care. Palliative care relieves suffering and improves quality of life for people of any age and at any stage in a serious illness. Palliative practices are present whether the illness is curable, chronic or life threatening. Our palliative care practices provide each patient and their loved ones with respect, dignity, and an individualized care plan that meets their specific needs.
Pediatric Oncology Clinic
Pediatric Oncology Clinic
- T 905-895-4521, ext. 2231
Stronach Regional Cancer Center, level 1
Southlake’s Pediatric Oncology Satellite Clinic is located on Level 1 of the Stronach Regional Cancer Centre. We deliver cancer care for children, from birth to 18-years-of-age, through our partnership with the Pediatric Oncology Group of Ontario (POGO) and SickKids Hospital. Our nurses, pediatricians, pediatric oncologists and interprofessional members work in partnership with similar teams at SickKids to provide quality care closer to home.
To learn more about the POGO Pediatric Oncology Satellite Clinic at Southlake, click the image below.
Psychosocial Oncology Program & Clinics
Psychosocial Oncology Program & Clinics
Psychosocial oncology is a whole-person approach to cancer care. Our Psychosocial Oncology Program team has specialized training and expertise in oncology. Depending on your needs, your team may include a combination of: registered dietitians, a medical psychotherapist, nurses, nurse practitioners, pharmacists, psychiatrists, and social workers.
We offer you a range of clinics and support group programs to improve your quality of life throughout your treatment and beyond. Clinics are held on Level 1, and most support group programs are held in our large meeting room on the Lobby level of the Cancer Centre.
Radiation Program Clinics
Radiation Program Clinics
- T 905-830-5800
Stronach Regional Cancer Centre
Radiation therapy uses high energy x-rays to damage and stop cancer cells from growing. Getting radiation is like having an x-ray — you will not see or feel anything, and you won’t become radioactive. Watch the following short video to learn about radiation therapy at Cancer Centre and what to expect.
Your radiation therapy involves the following steps, which all take place on the ground floor (G) of the Cancer Centre:
1 – Pre-Radiation Patient Appointment – You will attend a 20-minute, one-on-one education appointment with a radiation therapist to tell you what to expect at every step.
2 – Planning Appointment – You will attend a one-hour planning appointment, where you will be given a computed tomography (CT) simulation. This appointment will give your radiation oncologist and radiation therapist the information they need to accurately outline your treatment area.
3 – Treatment Delivery Appointment – You will go to the Ground Floor for your radiation treatment. Your first treatment will be the longest (30 – 45 minutes). We will monitor you throughout your treatment and during weekly visits with your care team.
Support Group Programs
Support Group Programs
- T 905-895-5800
You may experience potential challenges at various stages of your patient experience, such as forgetfulness, shortness of breath, stress and wondering how to get your life back on track. We offer various support group programs to help you address these challenges, as well as a bereavement program to assist those who have lost a loved one. To learn more about these group support programs or register for one, speak with a member of your care team.
Brain Fog
An eight-session support group program to help you deal with changes in your memory, managing tasks and improve your well-being during or after your treatments.
Pathways to Wellness
A six-session support group program to help you prepare for life after you finish your treatments.
Look Good Feel Better
As part of Canada’s “Look Good Feel Better” charity program, this one-session workshop gives you strategies and tips to help you manage changes in your appearance during or after you finish your treatments.
Mindfulness Based Stress Reduction, Cognitive Therapy, Insomnia
These support group programs teach you mindfulness meditation and other coping skills.
Thoracic Surgery School
Thoracic Surgery School
In preparation for thoracic surgery (surgery to treat diseases of the chest and lungs), patients are referred to Thoracic Surgery School by their surgeon. A qualified team of nursing, physiotherapy and pharmacy representatives conducts this outpatient service. It includes an overview of the anatomy and function of the lungs, the location of incisions, breathing and coughing exercises, pain control management, and the importance of early mobility. Following surgery, patients reconnect with their Thoracic Surgery School physiotherapists in order to receive post-operative rehabilitation.
Frequently Asked Questions
I feel scared and anxious, what support is available to me?
I feel scared and anxious, what support is available to me?
At the Stronach Regional Cancer Centre (SRCC) at Southlake, we know a cancer diagnosis may affect many aspects of your life: physical, financial, emotional, occupational, and spiritual. If you have been diagnosed, remember that you are a person who happens to have cancer. Cancer is not who you are and it does not define who you will be. It is normal to feel scared, anxious or unsettled when diagnosed with cancer.
You might find that you are worried about your emotional well-being, or you may have worries about finances or transportation.
That’s why it’s as important for you and your family to receive emotional, spiritual and social guidance, as well as your radiation or other treatments. At the SRCC at Southlake, we’re here to help every step of the way.
Radiation therapy: Are there any side effects from my radiation treatments?
Radiation therapy: Are there any side effects from my radiation treatments?
There are common side effects associated with radiation therapy, as it’s hard to destroy cancer cells without damaging some normal cells too. These side effects vary depending on the area being treated, the prescribed radiation dose and the length of your overall treatment.
Your radiation oncologist and radiation therapists will discuss any possible side effects with you and provide methods for managing them. The SRCC at Southlake also offers classes and information sessions to help you manage your side effects. We will also monitor you throughout your treatment and during weekly visits with your healthcare team.
Radiation therapy: Can I move around when the radiation is on?
Radiation therapy: Can I move around when the radiation is on?
Remaining as still as possible is important when the radiation is on. Relax and breathe normally. If you need to cough, don’t be polite and cover up. Cough straight up or down, depending on your position and you will naturally relax back into the correct position.
Radiation therapy: How close will the machine be to my body?
Radiation therapy: How close will the machine be to my body?
The machine will not touch you. It may move close to your treatment area, but it will not make contact with your skin.
Radiation therapy: will getting a tattoo hurt?
Radiation therapy: will getting a tattoo hurt?
You will feel a slight pinprick as a fine needle is used to place the tiny tattoos. Remember to relax and communicate with the staff about any concerns you may have.
Radiation therapy: Will I be alone when the treatment is being delivered?
Radiation therapy: Will I be alone when the treatment is being delivered?
Yes, once you have been placed into position, your radiation therapist will deliver your treatment from outside the room. Your treatment room has cameras and an intercom system, so staff will be able to see and hear you at all times. If you require assistance, feel free to call out and they will assist you, as needed.
Radiation therapy: Will I become radioactive?
Radiation therapy: Will I become radioactive?
No, just like taking an x-ray, once the radiation is turned off, radiation does not stay in your body. It is safe to be around family and friends while you are undergoing your treatments.
Radiation therapy: Will I feel any pain during treatment?
Radiation therapy: Will I feel any pain during treatment?
No, radiation is similar to having an x-ray taken. There is no pain or any sensation involved.
Radiation therapy: Will I see, feel, or hear anything while receiving my radiation treatment?
Radiation therapy: Will I see, feel, or hear anything while receiving my radiation treatment?
You will not see or feel anything during treatment. You will only hear noises from the radiation machine.
What kind of clinics and support groups are available to patients and families?
What kind of clinics and support groups are available to patients and families?
We offer you a range of clinics and support group programs to improve your quality of life throughout your treatment and beyond. Clinics are held on level one (1) and most support group programs are held in our auditorium on the lobby level of the SRCC at Southlake.
To hear about the SRCC at Southlake’s supportive care clinics and programs that can help you, watch the less than two-minute video below.
What support is available if I am not able to visit my loved one in person?
What support is available if I am not able to visit my loved one in person?
If you would like to arrange a virtual visit with your loved one please email the patient’s name and your contact information to VirtualVisit@southlake.ca.
Who will be part of my care team?
Who will be part of my care team?
Depending on your needs, your team may include a combination of: registered dietitians, a medical psychotherapist, nurses, nurse practitioners, pharmacists, palliative care physicians, physiotherapists, psychiatrists and social workers.
We have recently rolled out an end-of-shift check in pocket card for all staff, adapted ...
Apr 24
We’re celebrating Patient Experience Week! A time to recognize healthcare staff impacting the patient experience ...
Happy #NationalNursingWeek to the many amazing nurses and other heroes of @southlakerhc who are working ...
Apr 22
RT @DeputyPDaSilva: I am humbled & honoured to be the Executive Sponsor for the @YRP ...
Southlake staff want to say thank you, to YOU! Through donations such as meals and ...
Apr 22
An AMAZING accomplishment! Thank you for your unwavering support for the doctors, nurses, allied health ...
We are thrilled to announce a new community initiative to raise funds for Southlake's COVID-19 ...
Apr 22
Thank you for being heroes in the fight against childhood cancer @YRP @CentralYorkFire @YorkParamedics… https://t.co/sChkZa5jCJ ...

